In cases where the patient’s symptoms do not improve with conservative treatments, minimally invasive interventionist techniques are used. The most frequently chosen option is thermal radiofrequency ablation (rhizolysis), which consists of performing a controlled lesion to the medial branch of the posterior root of the corresponding spinal nerve. This controlled nerve injury is provoked by a local increase in the vibration of the particles surrounding the active tip of the cannula. Between 60-90% of patients experience significant improvement in pain.
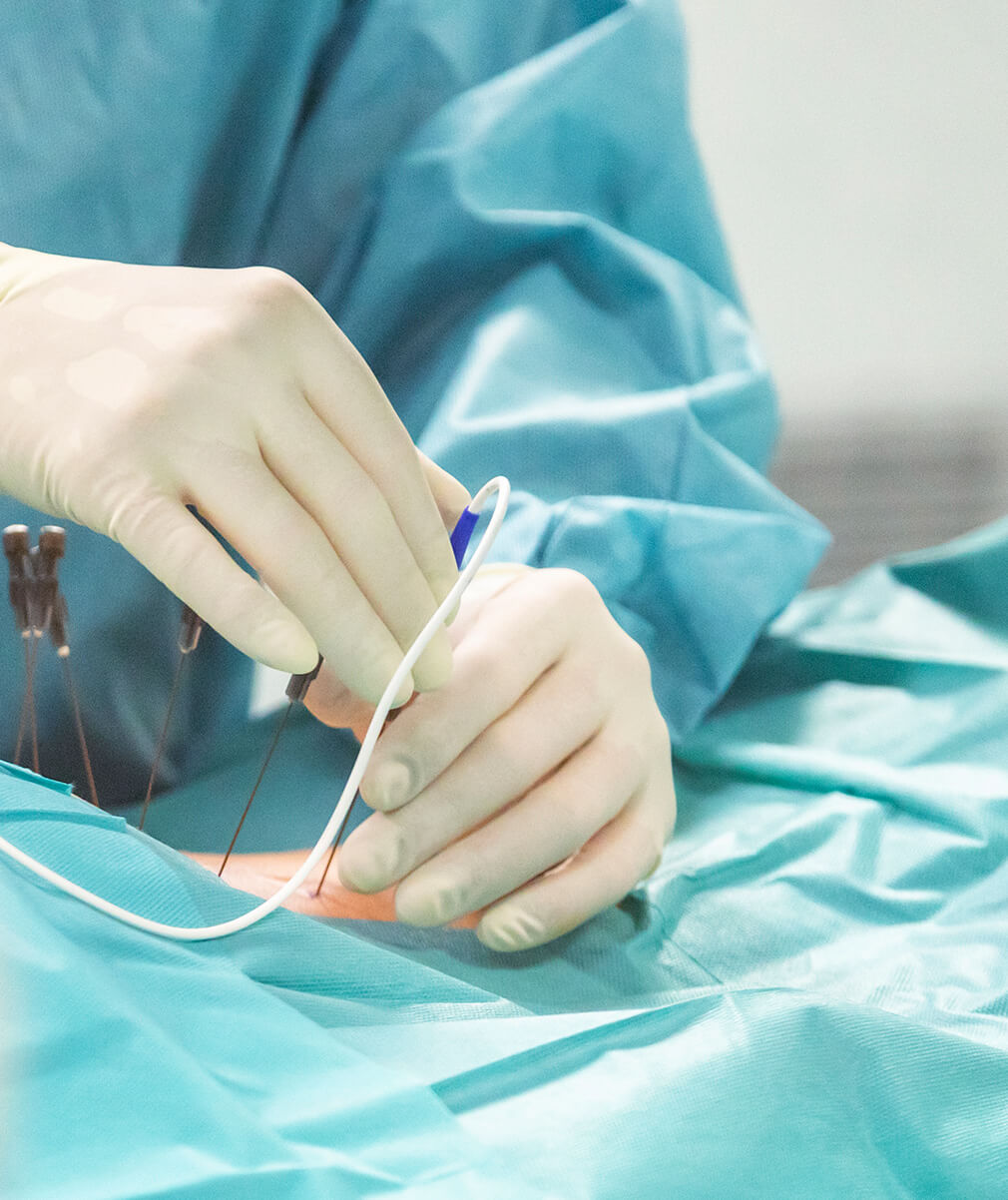
The minimally invasive technique of joint injections is performed in an operating room, with light sedation that allows patient collaboration. The entire procedure is monitored with a fluoroscope. A needle with a sensor in its tip is inserted into each of the affected joint or joints.
First, a sensory check is performed (50 Hz), followed by a motor check (2 Hz), in which we do not want to see root stimulation, although fasciculations may appear. Once the safety of the procedure has been verified, the radiofrequency is started. There are two types, the conventional one, which uses heat at 80ºC for 60-80 seconds, or the pulsed one, which is usually carried out for 120 seconds and reaches temperatures of 40-42ºC.
This minimally invasive technique can be performed on the entire spine from the cervical area (starting at C2) to the lumbar and sacral area. In addition, it can be unilateral or bilateral, depending on the patient's situation. Most patients experience immediate improvement, although this may not be noticed until up to 4 weeks after the procedure.
It is considered a safe technique, with a low rate of complications. Despite this, there are patients who experience pain or discomfort in the operated area, and there have even been cases of nerve pain in the form of a burning sensation or dysesthesia, which improves within 4-8 weeks afterwards.
It should be noted that the neural blockage achieved lasts for a given period of time, and the pain may reappear again. It is difficult to predict how long the pain relief from this treatment will last for each patient, since it can vary from 6 months to several years. It is good to know that if the facet joint pain reappears, the facet joint injections can be performed again.