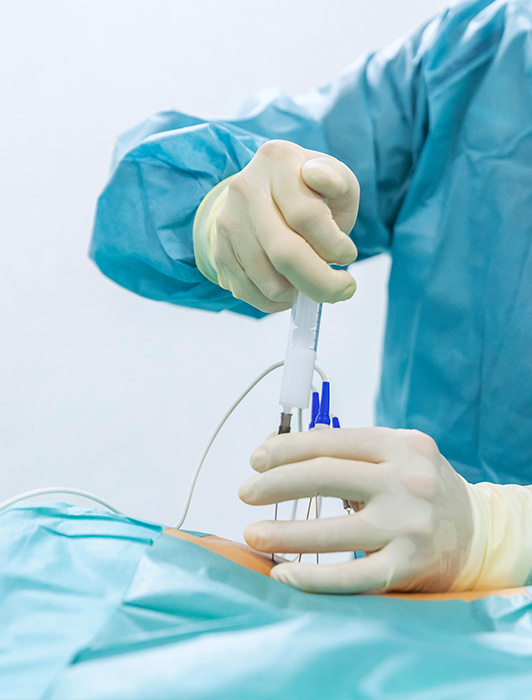
The following approaches can be used to perform the infiltrations:
- Interlaminar: the corticosteroid is deposited in the posterior epidural space and is not considered to directly reach the cause of the problem, that is, the anterior epidural space. An interlaminar approach can be performed by accessing the ventrolateral EE with a catheter.
- Caudal: this approach requires more volume when away from the nociceptive pain focus, although it is an easy technique and with fewer risks.
- Trasforaminal: This technique has grown more popular as fluoroscopy has become more widely used, making it possible to deposit the concentrated corticosteroid in the intervertebral foramen and pass it to the ventrolateral epidural space, where the focus of pain is around the inflamed root.
In the past, interlaminar and caudal techniques were always done blindly. However, there are several studies showing that blind epidurals performed by experts fail in the correct location of the space up to 30% of the time. To improve this, it is currently recommended that all procedures involving an epidural approach be performed under fluoroscopic control in operating rooms or rooms prepared with resuscitation material and performed by experts who can recognize and treat the potentially serious complications of these techniques.
1. INTERLAMINAR LUMBAR EPIDURAL
The patient lies face down with the head to one side, in a slightly flexed position with an abdominal pillow to improve flexion of the spine and better visualize the epidural space.
After choosing the level, a medial or paralaminar approach can be tried, entering the ipsilateral epidural space on the affected side. Sedation should not be used, or it must be very light. The sterile needle is inserted, trying to find loss of resistance, checking frequently by x-ray.
In practice, up to three infiltrations are usually made, with 1-4 weeks of space between them. Some patients may not respond with three infiltrations and may respond with a fourth. If 100% relief is obtained after an infiltration, the following is not performed. Doses are reduced in elderly or diabetic patients.
2. CAUDAL EPIDURAL
This approach is performed under the same conditions as the interlaminar, and enters through the sacral hiatus. It is generally not difficult to enter through this hiatus, after palpation of the two sacral horns and traverse the sacrococcygeal ligament. The position is monitored with contrast with the lateral position x-rays. To reach the affected level (generally L5-S1 or L4-L5), it is necessary to use a greater volume of medication than for an interlaminar infiltration.
3. CERVICAL EPlDURAL
The same technique is used as for the lumbar epidural, although some authors prefer to do it with the patient seated, and always guided by x-ray imaging. In this procedure, it is easier to reach the anterior epidural space with the injected liquid than in the lumbar area, which is the reason that cervical epidurals tend to be more effective.
This intervention is safer to perform at the upper thoracic levels, by inserting the epidural catheter to the affected level. X-ray imaging in the lateral position is very complicated because of the superimposition of the images of the shoulders, so oblique projections are used.